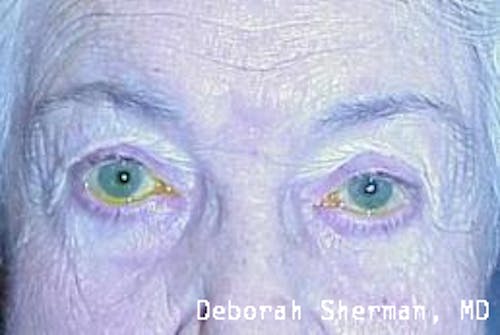
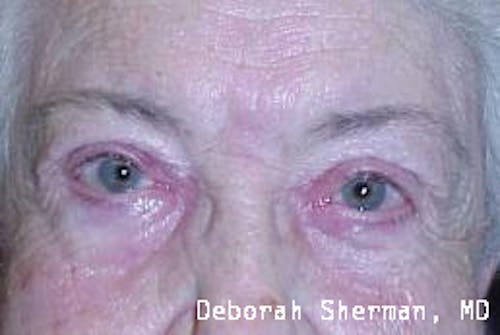
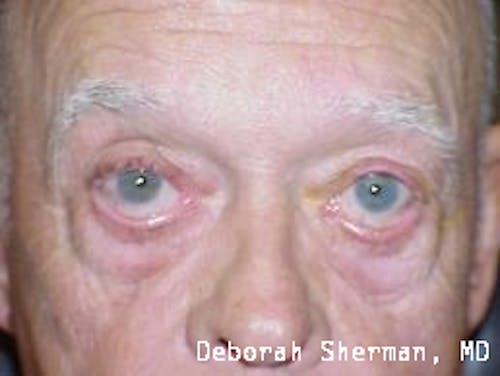
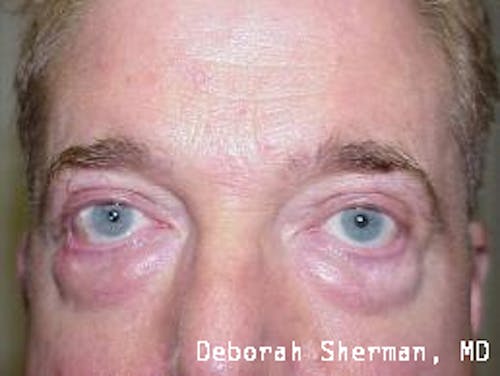
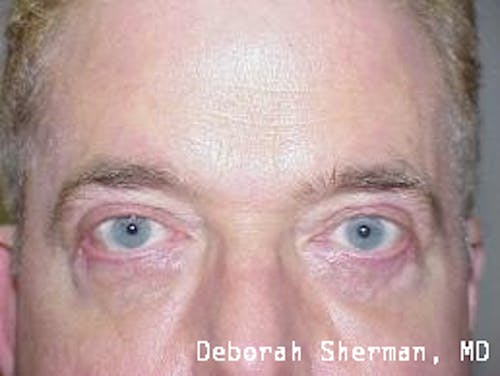
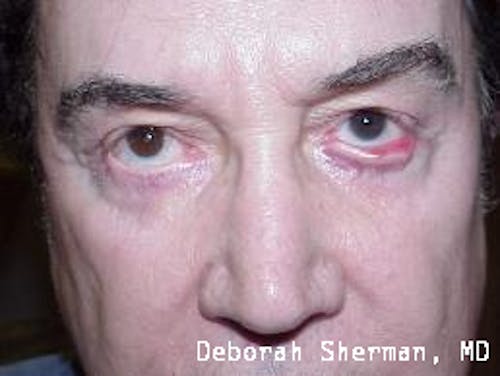
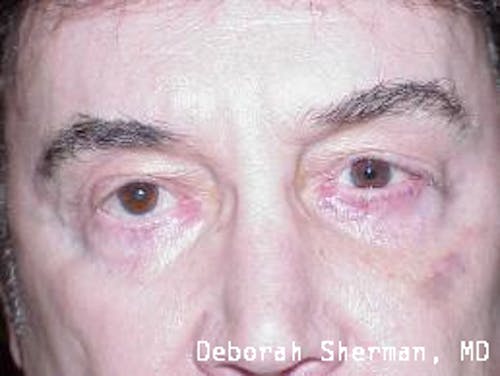
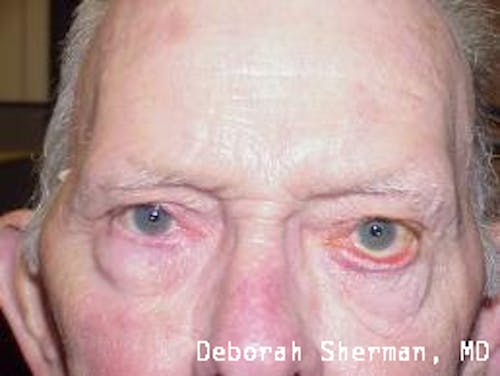
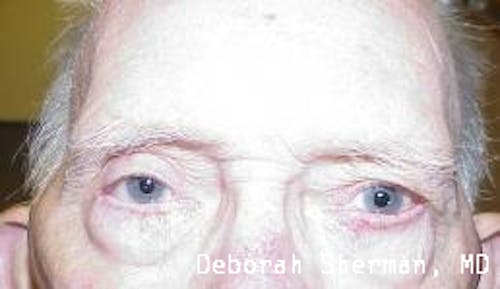
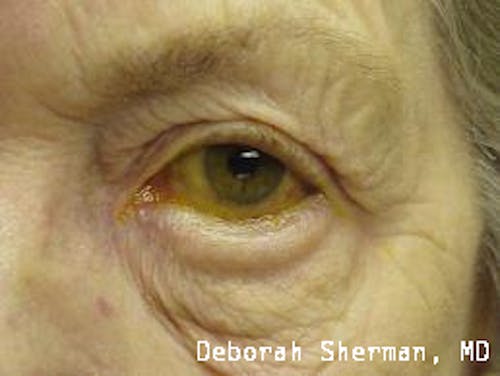
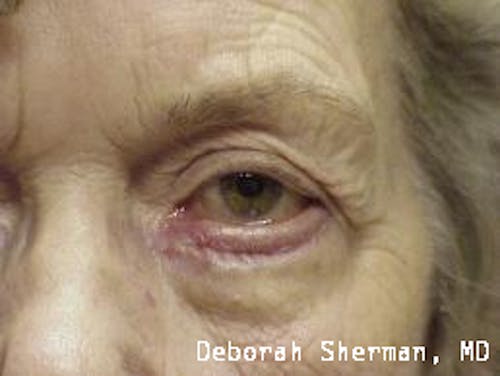
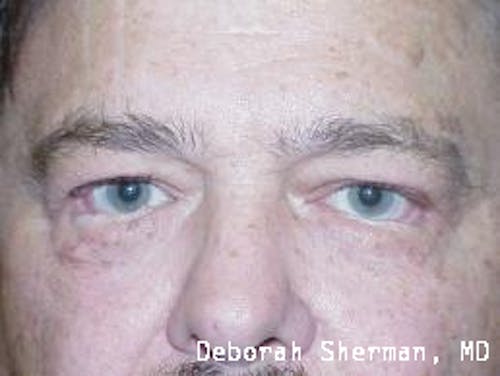
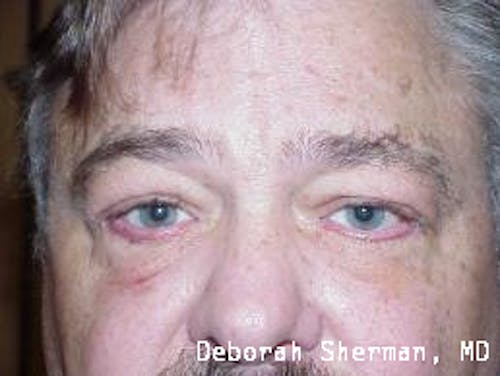
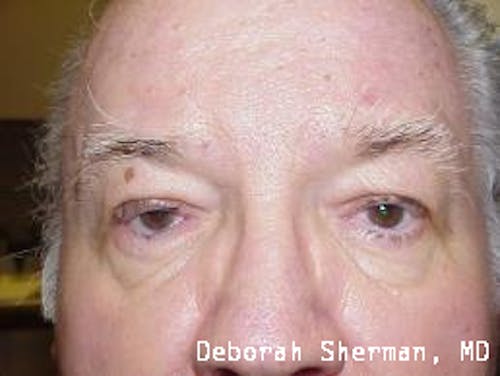
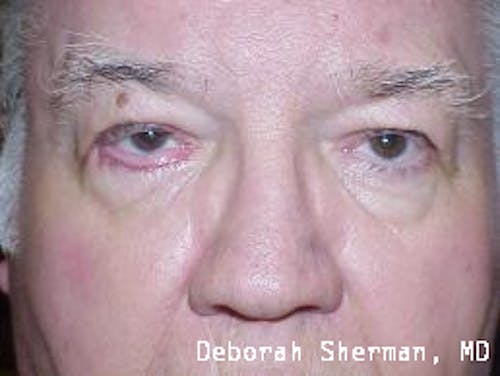
See the Nashville, TN, expert for eyelid malpositions, such as ectropion and entropion.
What Is Eyelid Malposition?
The supporting structure of the lower eyelid may be likened to a hammock, with an inner layer of a cartilage-like element (tarsal plate) that gives the eyelid stiffness and helps the eyelid stay in proper position so it functions normally. Each end of the eyelid hammock attaches two tendons to the bone on either side of the eye. If these tendons become too loose, the eyelid may turn outward or inward. Ectropion is when the eyelid turns outward and can cause excessive tearing or dryness and irritation of the eye. Entropion is when the eyelid turns inward, which can cause the eyelashes to irritate the eye.